Knowledge Center
August 23, 2024
The Complete Guide to Surgical Lights
What are Surgical Lights?
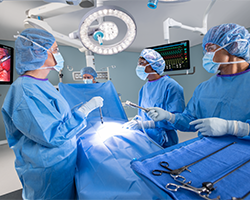
Surgical lights, also known as surgical lighting or operating lights, are mainly used in hospital operating rooms (OR) and ambulatory surgery centers (ASC). Surgery lights can also be used in various locations throughout the facility to provide high-quality lighting for procedures. Examples include emergency rooms, labor and delivery, examination rooms, and anywhere where procedures are completed. Clinicians, surgeons, and proceduralists use them. A surgical light illuminates the operative site on a patient for optimal visualization during a procedure.1 Surgical lights can provide hours of bright light without excessively heating the patient or staff. Various lights are available to provide optimal visualization during surgery and procedures. An examination light is used during medical exams, while operating room lights are used during surgical procedures.
History of Surgical Lights
Before electricity allowed lightbulbs to illuminate an operating room, candles were used as a light source during a procedure. Additionally, surgeries were performed during daylight hours so surgeons could use the natural sunlight for illumination.2 Surgical lights, as recognized today, have evolved over a century since electricity was first discovered in 1879, with surgical light manufacturers continuously working to improve lighting conditions for surgeons and OR staff.
Types of Surgical Lights
There are various types of surgical lights, and each type plays specific roles in illumination before, during, and after a medical procedure. They can be categorized by lamp type or mounting configuration. Two common types of lamps are conventional (incandescent) and LED (light-emitting diode) lamps.
Surgical lighting configurations may include ceiling-mounted, wall-mounted, or on-floor stands. Depending on the model, a surgery light may also be used in all three configurations.1 A ceiling-mounted light can be mounted on a fixed point on the ceiling of a procedure room. The low-profile LED202 In-Ceiling Lighting System is designed to provide comfortable, high-quality illumination that can be adjusted to meet various clinical needs. A below-ceiling dome offers 56 degrees of lighting articulation for optimal aiming and versatile installations in any clinical setting.
Similarly, wall-mounted lights are mounted on a wall of the OR. The wall-mounted configuration is more often used with examination lights than surgical lights. For greater mobility, floor-standing surgical lights are standalone and typically on wheels, enabling them to move from room to room. Mobile floor-standing lights are often used in examinations. All three types play an important role in illuminating a surgical site during a procedure.
Explore our Surgical and Examination Lights
Incandescent Lighting
Halogen bulbs were historically considered conventional surgical lights and utilize a type of incandescent bulb filled with halogen gas to produce light inside the lamp. Halogen enables the filament to run at a higher temperature because, although the tungsten is evaporated off the filament faster at the higher temperature, the halogen chemically reacts with the evaporated tungsten to form a tungsten halogen compound, which diffuses back to the filament where the higher temperature causes it to separate into tungsten and halogen, depositing the tungsten back on the filament.6,7 Their lower filament-correlated color temperature at 3,000K gives them their typical orange-yellow, warm-appearing cast rather than white.
Standard halogen lights have an average short life span of approximately 1,000 to 3,000 hours and often die abruptly.8 When lit 24 hours a day, seven days a week, this translates into about six months of life. Changing bulbs every six months can become costly to an organization over time. If halogen lamps are touched with bare hands, even when cool, the oil from the person’s fingers can heat, shortening the bulb's life. They emit a substantial amount of heat, making them hazardous to touch, especially when turned on, and uncomfortable to work under while performing a procedure. The high-pressure gas combustion properties necessitate a shield to protect users in many environments if the bulb shatters.9 They produce relatively low luminous efficacy, and often, perioperative teams must turn them up to full intensity to get adequate illumination. Their low luminosity is worsened by filters that must be used to reduce the amount of non-visible radiation they emit.8 Infrared and ultraviolet rays produce radiation that poses a potential threat to the health of patients and the perioperative team. Also, non-tunable CCT, low efficiency, and short lifetime indicate that halogen lamps may not be the best solution for surgical lighting.7,10 They can facilitate a dangerous environment where there is a risk of getting burned if perioperative staff accidentally come into direct contact with them, and excessive heat was such a significant issue that ORs invested in the added cost of heat protection filters.
The glare from halogen lights became a risk as it caused fatigue and eye strain when surgeons looked away from the surgical site into glaring lights and needed time for their eyes to adjust when refocusing their attention on the surgical cavity. In fact, in the early 1900s, some surgeons began using dark-colored cloth and sheets during surgery to minimize glare. The black cloth did not allow for immediate assessment of clean versus soiled linen, so eventually, the standard became to use green linen to reduce glare and allow for the visualization of soiled material.11 In 1914, Dr. Harry Sherman introduced green linen and décor into the ORs because he found that green reduced glare from lighting and complemented hemoglobin red, the color of blood, to allow for greater procedural visibility. He discovered that his eyes could rest on the details and texture of the surgical cavity without competing with the ambient light. Soon, several other surgeons followed this direction.11,12
Tungsten-Halogen Lighting
Tungsten Halogen lighting is an incandescent light with a filament inside the bulb filled with halogen gas. The filament of a Tungsten Halogen Lamp has two purposes: to generate light and the heat necessary to obtain a wall temperature exceeding 250°C. The combination of Tungsten and halogen gas produces a chemical reaction, redepositing evaporated tungsten on the filament. The process allows the filament to operate at a higher temperature and produce light with higher efficacy and color temperature.18
LED Lighting
In the early 2000s, LED became a standard offering in many industries, including ORs and other procedural areas,13 and surpassed conventional halogen light sources as the preferred light source used during surgical procedures.14 They are solid-state semiconductor devices that emit light as currents flow through them. They have a more refined energy usage and require significantly less energy than a halogen to produce equal to higher quality illumination. The plastic encapsulant and the lead frame compose most of the bulb’s structure, and the light-generating chip is comparatively small. Light is generated inside the chip, a solid crystal material, when current flows across the junctions of different materials. The spectral emission of the LED light depends on the materials used to form the semiconductor, the most common combinations being aluminum indium gallium phosphide and indium gallium nitride.6 The composition of the materials determines the wavelength and color of the light (i.e., red, yellow, green, blue, or white). Initially, LED surgical lighting used a combination of red, green, blue, and white LEDs to achieve a bright white illuminance. This strategy was the primary means to achieve high light output superior to what using all-white LEDs could produce. Unfortunately, the light would change color when a hand is placed in the sterile field, which blocks one or more colors.
LEDs can be extremely small, durable, reliable, and have a much higher bulb-life rate than conventional lighting. The current determines the light output of LEDs through the semiconductor and its temperature. LEDs can have a long life of up to 60,000 hours when using the maximum current recommended by the manufacturer.6 However, most are generally rated for 25,000 to 40,000 hours of full light, and rather than failing abruptly like halogen bulbs, they gradually fade in brightness. In terms of luminous efficacy, LED lights used during procedures typically do not require a filtering media, as is needed with halogen surgical lamps, which contributes to their relatively low luminous efficacy. LEDs offer higher efficacy, allowing for reductions in connected load of 50% or more, virtually eliminating the problem of infrared radiation caused by excessive heat, with the potential for additional energy savings through constant-color dimming and reduced cooling load in the OR.8 The latest LED products are high-flux and have luminous efficacies up to 100 lumens per watt (lm/W) and higher.6 Because past OR practices involved turning lights up to full intensity, original perioperative staff would do the same with LED lights. Unfortunately, this created distortion. To avoid distortion, standard practice begins at a 50% intensity level. Many surgical lamps offer enhanced properties to mitigate shadows cast by the surgeon and perioperative team; some products also allow color adjustment.8 Their availability in a wide range of spectral power distributions (SPDs) permits the development of spectrally tunable surgical luminaires, where an array of LEDs with distinct SPDs can be mixed to produce a variety of spectra from a single luminaire.15
High-Intensity Discharge (HID) Lighting
Gas-discharge lamps generate light by sending an electrical discharge through ionized gas. High-intensity discharge (HID) lights are electrical gas dischargers that use an electric arc to produce intense light. Like fluorescent lights, they also require a ballast. They provide the most extended service life out of all lighting types. HID surgical lamps are commonly used for outdoor lighting and in large indoor areas. They are most suitable for applications that stay on for hours.1
The three most common types of HID lights are:
- Mercury vapor lamps
- Metal halide lamps
- High-pressure sodium lamps
Since most HID lamps produce light that is either very cool white/blue or warm white/yellow, they are generally not used in applications where the aesthetic quality of light is essential. Also, some HID bulbs require an extended warm-up time and are unsuitable for applications where lights are turned on and off regularly.
The different types of light
The primary function of surgical lighting is to illuminate the operative site on and/or within a patient for ideal visualization by OR staff during a surgical procedure. With proper lighting, operating room staff can achieve a higher level of efficacy during surgery and reduce the risk of complications.16
Specular
Specular lighting stimulates the bright spot of a light that appears on shiny objects, such as surgical instruments. Specular highlights are more inclined to the color of the light than the color of the object it appears on. This light retains its reflective qualities.2
Diffused
Diffused lighting stimulates the directional impact a light object has on an object. This is the most visually significant component of the lighting model. The more a part of an object faces the light source, the brighter it becomes.
Diffuse lighting is brighter the closer its fragments are aligned to the light rays from the light source.2
Requirements for Surgical Lights
Surgical light requirements vary depending on the lighting system's type, brand, and model. The brightness of a surgical lighthead is measured in Lux and typically does not exceed 160,000 Lux. The approximate dimensions are 400-700mm for a lighthead diameter, and the approximate weight is 45kg. The weight can vary depending on the number of lightheads attached to the system. The lifespan of a surgery light is measured in its L70 value, which is how long the light will last until its brightness is 70% of its original value. Today's surgical lights typically last between 40,000 to 60,000 hours of use.
Operating Room Lighting Methods
Quality lighting is vital for every OR; the lighting method depends on the needs of the staff and patients. Three of the most common methods are:
- Overhead/operating lights
- Headlights/illuminated loupes
- In-cavity lighting
Overhead/Operating Lights

Overhead lights are typically LED or incandescent and can be mounted on a ceiling or wall. These operation room lights have handles that allow the surgeon and perioperative team to adjust the lighting for the best visualization, helping to prevent glare and optimize surgical site visualization.
Challenges with overhead lighting include the potential for not precisely illuminating the surgical site, resulting in the operative site being flooded with large amounts of light that do not permit exact spot patterns to see far and wide into the cavity.4 This can create a diffused light pattern with strategic lenses.
ALYON™ Surgical Lighting System offers precise illumination and adaptive lighting for superior optical performance for ORs and ASCs. This surgical light has ten different intensity settings, four spot sizes (focal point sizes), and four different color temperature options, with 160 ways to customize your lighting experience.
The HarmonyAIR A-Series Surgical Lighting System redefines optical performance through excellent color, contrast, clarity, and control. A unique peninsula design provides optimal illumination at the surgical site, including deep cavity procedures. You can automatically maintain constant light intensity even when the light is adjusted or moved during a procedure.
Headlights/illuminated loupes
Headlights are wearable technology that provides brightness, dependability, and small spot size for surgeons by enabling light to follow the surgeon's attention and enhance mobility and shadow-free illumination. These headpieces can be battery-powered or connected to a standalone light source with a fiber optic cable. Headlamps can be uncomfortable, resulting in head and neck pain after an extended period. When connected to fiber optic cables, movement is limited, requiring the surgeon to detach the cord for the light source and reattach it as it moves around during the procedure. They can also increase clutter and become a tripping hazard in the OR.16
Battery-powered headlights come in several options. Most still use a cord going from the headlight to a battery pack clipped to the waist of the user. This can cause pulling pressure on the back of the neck. Over time, this pressure can cause neck pain and headlight illumination to shift on the head of the user, requiring adjustment throughout the procedure. This has been the usual design because the weight of batteries precluded them from being integrated into the headlight. New technology allows for a truly cordless headlight. Headlights with very lightweight batteries that are balanced on the user’s head are the best option for removing all cords associated with headlights. Design with the user in mind will also provide comfort bands that do not squeeze the user’s head. This can be a cause for headaches and neck pain. Over time and repeated uses, this can become cumulative and result in chronic musculoskeletal conditions.
Headlights are necessary adjuncts for deep, lateral, or narrow surgical sites. Many surgeons report using them most of the time, even 100% of the time. With this amount of usage, assessing the comfort, weight, performance, and battery life is worthwhile. Performance includes the amount of light measured in LUX, the spot size range, and the ease of use.
Illuminated loupes are small magnifying devices typically attached to surgical glasses' lenses or frames. Many surgical loupes contain a small lamp attached to the center of the frame to illuminate the operative site. These lights are critical in some cases because they enhance and magnify an area during surgeries requiring a high level of dexterity when working with small body structures.16
In-cavity Lighting
In-cavity lights enable illumination deep inside surgical cavities. In-cavity lighting is a practical option if current overhead and headlamp lighting are inadequate. This light source is generally fixed on its own or attached to a surgical instrument outside of the sterile field or combined with fiber optics to eliminate factors such as added heat.16
This type of lighting is only practical for some surgical cases. First, in-cavity lighting can be cumbersome and emits very little light. It can also become an infection risk because it is another item placed inside the patient and requires larger incisions, whereas modern surgery endeavors tend to be minimally invasive.
Choosing the lighting for procedures
Surgical lighting is one of the most critical factors in the OR environment. The type of surgery performed tends to influence the surgical lighting needed. Without the correct light source, the surgeons’ risk of making mistakes increases and could affect the following:
- Surgery outcomes
- Increased malpractice claims
Surgeons need the correct light source that maximizes visibility and efficiencies in the OR. 5
Lighting for Open Surgery
Traditional open surgery can utilize overhead lighting when the operative site is not deep within the patient. LED lighting is the most conventional light source used for open surgery. Emphasizing the reduction of shadows is crucial for open surgery. Obstructions are expected between the light source and the surgical site, i.e., head, shoulders, hands, instruments, etc.
Lighting for Minimally Invasive Surgery
In-Cavity Surgical Lighting
In-cavity surgical lighting emits minimal lighting and is best used during minimally invasive applications. The light source is outside the sterile field, often fixed on a surgical instrument, allowing the supplement of overhead and headlamp lighting in non-invasive surgical procedures. Heat management is the most critical factor when using in-cavity lighting fixtures.3
Surgical Microscope
A surgical microscope, also known as an operating microscope, is an optical microscope specifically designed for microsurgery. The surgical microscope provides adjustable magnification, bright illumination, and clear visualization of the surgical field and has been used more progressively in operating rooms. State-of-the-art surgical microscopes are integrated with various imaging modalities, such as optical coherence tomography (OCT), fluorescence imaging, and augmented reality (AR) for image-guided surgery. The surgical microscope is a powerful tool that can offer optional magnifications, bright illuminations, and clear visualization.17
Lighting for Laparoscopic
In-Cavity Lighting (coupled with In-Cavity Imaging)
In-cavity lighting is best used for minimally invasive procedures. This process garners its name from the laparoscope, a tiny tool with a video camera and a light at the end of it. It involves less cutting and internal scarring. Products will often use highly targeted methods of transmitting lighting (fiber optics are often used) to illuminate the inside of a surgical cavity. These tools utilize a light generator and then “pipe in” lighting into the cavity.
Surgical Lighting Accessories
Accessories for a surgical light can complement or add to a surgical light system after it is initially purchased and installed. Accessories can encompass many products, but certain ones are typically available when purchasing a surgical lighting system. Crucial attributes may include (but are not limited to) the ability to add ambient light to a surgical light mount, the ability to add a free-standing camera for recording and/or teaching purposes, the ability to add a single or dual monitor mount, or the ability to add a radiation shield. Other accessories may include sterile light handle covers that can be utilized to maintain a sterile environment where a surgeon still has control of the function and position of the position, intensity, and spot size of the light from the handle light.
Where to Buy Surgical Lights
Because surgical lighting is complex, sophisticated, and often customized for an operating room or examination room, purchasing this equipment can be a multi-step process. Ensuring a procedure room has the necessary type of surgical light or exam light is the main factor in performing successful and safe procedures. Staff purchasing equipment for their facility may consider factors like brand, service support, long-term and short-term cost, and environmental sustainability when deciding which surgical lighting systems to purchase. Typically, a sales representative or distributor helps to facilitate the buying process of operating room lights.
Summary
Surgical lights are essential to surgeons, proceduralists, and the perioperative team in providing optimal visualization during procedures. For decades, choosing operation room lights has been challenging, as the proper lighting is critical for optimum patient safety and staff comfort. Although some ORs may opt to invest in poor-quality lighting systems, they are also likely to bear the brunt of poor performance outcomes for the perioperative team and clinical outcomes for patients. Inadequate lighting is a safety hazard that can lead to injury if an object's position, shape, or speed is misjudged. It can affect the quality and precision of work—too much or too little light strains the eyes and may cause eye discomfort for staff. New-generation LED surgery lights can help solve these issues and create ideal conditions in the OR. LED systems emitting pure white light allow surgeons to assess and interpret the surgical cavity’s anatomical appearance accurately and consistently. Auto intensity functionality helps surgeons better discern between a spectrum of deep, saturated reds, precise contrast, and definition needed for superior tonal definition. A uniform beam eliminates hot and cold spots and reduces eye fatigue.
Article References
1 https://pdhonline.com/courses/e423/e423content.pdf
2 https://learnopengl.com/Lighting/Basic-Lighting
3 https://www.bfwinc.com/guide-to-surgical-lighting/
5 https://www.lumitex.com/blog/surgical-lighting
6 Boyce PR. Human factors in lighting. [PDF]. Crc Press; 2014.
7 Liu P, Zhang Y, Zheng Z, Li H, Liu X. LED surgical lighting system with multiple free-form surfaces for highly sterile operating theater application. Applied optics. 2014;53(16):3427-37. DOI: https://doi.org/10.1364/AO.53.003427
8 U.S. Department of Energy. Technical guidance document: LED surgical task lighting. Energy Efficiency & Renewable Energy Center. [PDF]. 2011.
9 Edison Tech Center. The halogen lamp. https://edisontechcenter.org/halogen.html. [Nd]. Accessed January 30, 2020.
10 Matern U, Koneczny S. Safety, hazards and ergonomics in the operating room. Surgical endoscopy. 2007;21(11):1965-9. DOI: https://doi.org/10.1007/s00464-007-9396-4.
11 Kisacky J. Blood red, soothing green, and pure white: what color is your operating room?. Color and Design. Bloomsbury. New York, NY. 2012:118-24.
12 Pantalony D. The colour of medicine. Cmaj. 2009;181(6-7):402-3. DOI: 10.1503/cmaj.091058.
13 Mulvaney D, editor. Green technology: an A-to-Z guide. London, UK. Sage; 2011
14 Knulst AJ, Stassen LP, Grimbergen CA, Dankelman J. Choosing surgical lighting in the LED era. Surgical innovation. 2009;16(4):317-23. DOI: 10.1177/1553350609353766.
15 Houser KW, Mundinger JJ. Surgical Luminaires with Adjustable Spectrum. Lighting Research & Technology. 2017. DOI: http://dx.doi.org/10.1177/1477153517742682.