Knowledge Center
November 7, 2023
How to Prevent Retained Surgical Items
Preventing Retained Surgical Items
In the fast-paced and high-stress environment of an operating room (OR), it's possible for small items like surgical sponges and gauze and surgical instruments to be left in a patient's body unintentionally. These retained surgical items (RSIs) can cause serious patient harm, including infection, organ damage, and even death. OR teams have relied upon manual counting processes to prevent RSIs; however, manual counting is easily interrupted throughout a complex procedure with competing demands, tasks, and possibly numerous participants, which can lead to errors. The introduction of new technology is making it quicker and easier to track items and prevent RSIs from occurring. In this article, you will learn about the following:
- Retained surgical items statistics, risks, causes, and the likelihood of occurrence
- The challenges that clinicians and hospitals face with RSIs, and
- How to prevent retained surgical items by adding technology to the counting process
Help Prevent Retained Surgical Items with ORLocate Surgical Counting and Detection System
What are Retained Surgical Items?
Retained surgical items, or retained foreign objects (RFOs), are medical devices, tools, sponges, or instruments unintentionally left inside the patient cavity after the surgical site is closed. There are a variety of reasons why RSIs occur. One of the primary causes is human error. This can happen due to gaps in communication among surgical team members, inadequate documentation of items used during the procedure, and even misplaced confidence or complacency from not having experienced this adverse event. Surgical staff may verify miscounts thinking they’re accurate, or they may overlook an item that has been left behind.
Though there are different types of RSIs, one of the most common is a surgical sponge. Retained surgical sponges alone account for nearly 70% of all RSIs. These sponges absorb blood and other fluids during surgery but can easily be missed during a manual count of surgical items during and at the end of a procedure. Counting makes up 14% of OR time on average and requires nursing staff to be focused on counting rather than assisting the surgeon with patient care. This is one of several reasons why introducing assistive technology to counting processes is recommended.
How Often Do Retained Surgical Items Occur?
The rate of RSIs has varied due to differences in reporting. A four-year study conducted at the Mayo Clinic in Rochester, Minnesota, found an incidence of RSIs occurring in approximately one in every 5,500 surgical procedures. Additional studies have estimated that nearly 1,500 cases occur in the United States annually.1 Surgery is demanding, with the risk factors of retained surgical items increasing, particularly in complicated cases such as patients with a high body mass index (BMI) or trauma requiring numerous instruments, retractors, and surgical sponges.
Although the incidence of a retained surgical item might be considered rare compared to the millions of operations performed worldwide, these sentinel events can significantly harm patients. A five-year review reported to the Joint Commission discovered that more than 69% of RSI cases led to unexpected additional care or an extended hospital stay. More than 14% of the events resulted in severe, temporary harm.2 Moreover, the consequences of retained surgical items are potentially life-threatening if not caught and allowed to remain inside the patient.
What is the Most Frequent Site of Retained Surgical Items?
RSIs are often reported in the patient cavity, waste bins, kick buckets, or the OR. The abdomen and pelvis are the most common patient locations where RSIs are found, but there have also been reports of retained sponges in the thorax, spine, head and neck, brain, and extremities. Sponges also may be retained in procedures involving natural orifices, such as the vagina or nose, in minimally invasive surgeries, and after vaginal births.1
The Importance of Preventing Retained Surgical Items
The consequences of retained surgical items may have a lasting impact on the patient and the healthcare facility. The potential effects of a sponge being retained after surgery or other procedure affect the patient’s bodily function, leading to hospital readmission, reoperation, and possibly death. An incidence of RSIs can also have a significant financial impact on healthcare facilities. The cost of retained surgical items outweighs the cost of equipment to help prevent them.
In a recent review, the Pennsylvania Patient Safety Authority estimated that the average total cost of care related to an RSI is about $166,000, including the cost of the hospital’s legal defense, indemnity payments, and surgical expenses not reimbursed by the Centers for Medicare & Medicaid Services (CMS). Another study estimated medical and liability costs to be $200,000 or more per incident.3 A retained surgical item is viewed as a preventable “never event,” and as such, healthcare organizations and providers are not reimbursed for additional care provided because of an RSI.4
For 2020, CMS included “foreign object retained after surgery” as one of the four reportable hospital-acquired conditions (HACs) – among 14 HACs for which Medicare does not provide reimbursement. Additional care is unreimbursed, and hospitals with a total HAC score greater than the 75th percentile of all total HAC scores (the worst-performing quartile) are subject to a 1% Medicare payment reduction.5 In many instances, RSI cases lead to malpractice claims where members of the entire surgical team, and the facility, can be held liable.
Why are manual counts insufficient?
Despite diligent efforts, human management of the prevention effort needs to be revised due to environmental and biological factors. Even with strict protocols, one study showed that approximately 30% of sponge counts needed to be reconciled or completed. Another study found that counting isn’t always sufficient and may be omitted in emergency procedures. The neurology of the human brain functions in stressful environments, especially the limitations presented when distracted or under duress, showing that manual processes alone aren’t enough. A blend of human intelligence and technology is a necessary redundancy to help improve accuracy and create a safer environment.
The Use of Adjunctive Technology for the Prevention of Retained Surgical Items
Despite the effectiveness of adjunct technologies, ECRI Institute estimates that only 20% of hospitals in the United States use them to supplement the manual counting process or to aid in detecting missing sponges. Although the cost has been cited as a rationale for not adding adjunct technologies, one cost analysis showed that using tagged sponges would only add $12 per procedure and about 1 minute or less to the procedure time. This calculation must be balanced against an estimated 18 minutes to locate a missing sponge or the unreimbursed costs associated with an RSI, which can add up to hundreds of thousands of dollars per occurrence if it results in litigation.6
Three main types of technologies exist that are designed to supplement manual counting:
- Counting systems based on unique identifying barcodes or data-matrix codes annealed onto the sponge.
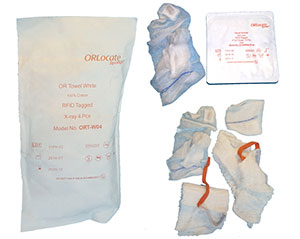
- Sponge-detection systems based on radio frequency (RF) tags that can verify the presence of a misplaced or unaccounted sponge.
- Counting and detection systems based on a radio frequency identification (RFID) chip embedded into the sponge.
Use of RFID Tracking Devices
RFID is a technology that uses radio frequency waves to detect identification tags attached to surgical items before a procedure. A reader placed near the surgical field detects RFID tagging, allowing staff to keep track of the location of each tagged item in real time. This technology has been used in various industries, including retail and logistics, but is now increasingly used in healthcare settings to prevent retained surgical items.
Adjunct RFID technologies can be used to find a tag in the open air, metal kick buckets, and patient cavities. Additionally, the serial number of each sponge, sponge description, and quantity of each type are recorded when scanned with technology capable of penetration and data transmission through tissue, such as high-frequency RFID.
What are AORN Guidelines for Preventing Retained Surgical Items?
The Association of periOperative Registered Nurses (AORN) has guidelines4 for preventing and managing retained surgical items. From a high level, these guidelines can be summarized in these key subjects:
- Counting: A "count" of all instruments and sponges should be conducted before, during, and after surgery to ensure that none are left behind. When a discrepancy in a count is identified, it is recommended that surgical team members act immediately.
- Identification and documentation: Any retained surgical items should be identified, removed, and properly documented.
- Use of radio-opaque markers: AORN recommends using radio-opaque markers on sponges and other items that may be difficult to detect on x-ray to aid in identification if they are retained.
- Reporting: Retained surgical items should be reported to the facility's risk management department, and the patient should be informed of the event.
- Continuing education and quality improvement: AORN recommends that perioperative staff receive ongoing education on the prevention and management of RSIs and that facilities implement quality improvement initiatives to reduce the incidence of RSIs.
Most recently, AORN guidelines have emphasized the involvement of technologies to help OR staff virtually eliminate RSIs.7 It’s important to note that these technologies aren’t designed to replace counting but rather to add to it. The counting process should not be completed when adjunct technology is used until the adjunct confirms the final count. Teamwork, communication, and perioperative planning are essential in preventing RSIs.
Contributors

Lena Fogle BSN, RN, CNOR
Senior Director Global Clinical Solutions, STERIS Healthcare
Lena is a seasoned healthcare leader with extensive experience leading complex perioperative environments as well as new program development, continuous process improvement, clinical outcomes, operational excellence, and stakeholder experience.
Related Resources
Article References:
1 Gawande AA, Studdert DM, Orav EJ, Brennan TA, Zinner MJ. Risk factors for retained instruments and sponges after surgery. N Engl J Med. 2003;348(3):229-235.
2 Steelman VM, Shaw C, Shine L, Hardy-Fairbanks AJ. Retained surgical sponges: a descriptive study of 319 occurrences and contributing factors from 2012 to 2017. Patient Saf Surg. 2018;12:20.
3 Joint Commission. Preventing unintended retained foreign objects. https://www.jointcommission.org/-/media/tjc/documents/resources/patient-safety-topics/sentinel-event/sea_51_urfos_10_17_13_final.pdf. Published October 17, 2013.
4 Association of periOperative Registered Nurses. Guideline for Prevention of Retained Surgical Items. In: Guidelines for Perioperative Practice. Denver, CO: AORN; 2019:765-816.
5 Centers for Medicare and Medicaid Services. Publicly reported DRA HAC measures: Frequently asked questions. 2020. https://www.cms.gov/files/document/frequently-asked-questions-publicly-reported-deficit-reduction-act-dra-hospital-acquired-condition.pdf.
6 TechNation Development Team. ECRI update: Retained surgical sponges are a top hazard, technology solutions can help. https://1technation.com/ecri-update-retained-surgical-sponges-are-a-top-hazard-technology-solutions-can-help. Published March 1, 2019.
7 Sadler D. New technologies help prevent RSIs.https://ortoday.com/new-technologies-help-prevent-rsis. Published February 1, 2012.






