Knowledge Center
October 15, 2020
The Ultimate Guide to the Trendelenburg Position
Positioning is imperative to patient safety during a surgical procedure. Proper patient positioning depends on the type and length of procedure, anesthesia access to the patient, devices required and other factors. While in Trendelenburg position, the patient is laid supine on the surgical table, and their head is angled down. This position, through the use of gravity, provides the surgical team with access to the patient’s abdominal organs by moving other organs in the abdominal cavity away from the surgical site.
What is the Trendelenburg position?
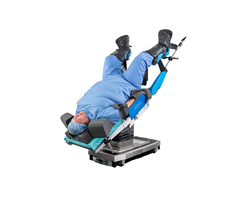
The Trendelenburg position is a position for a patient on the operating table, most commonly used during lower abdominal surgeries and central venous catheter placement. In Trendelenburg position, the patient is supine on the table with their head declined below their feet at an angle of roughly 16°.1 The degree of Trendelenburg should be minimized as much as possible, and if possible, the patient should be repositioned into the supine or reverse Trendelenburg position at established intervals.2 Due to the angle, the Trendelenburg position allows for the patient’s abdominal organ to move towards the head by the use of gravity, improving surgical access to the pelvic organs.
In steep Trendelenburg position, the patient is angled at 30 – 40 degrees in the head-down position. This version of Trendelenburg is most often used for robotic pelvic procedures. Risks associated with steep Trendelenburg position include altered pulmonary function, airway edema, increased intracranial and intraocular pressure, and nerve injury.3
When would you put a patient in the Trendelenburg position?
Trendelenburg position is typically used for lower abdominal surgeries including colorectal, gynecological, and genitourinary procedures as well as central venous catheter placement.
Considerations for Trendelenburg Position
When positioning a patient in Trendelenburg, surgical staff should consider various factors, including risk factors, potential for injury, and clinical recommendations for repositioning.
Brachial Plexus Neuropathy – The approximation of the clavicle and first rib threatens compression of the subclavian vessels and brachial plexus. Shoulder braces are causal to brachial plexus neuropathy: Gravity pulls the patient’s weight against shoulder braces, causing the shoulders to yield to pressure and body mass slides between the braces.
Perioperative complications from extreme Trendelenburg positioning – Keeping a patient in Trendelenburg for a long period of time may lead to a risk in various injuries, including ocular trauma due to increased blood pressure in the head including corneal abrasion, retinal detachment, ischemic optic neuropathy, as well as respiratory distress.
Clinical recommendations for repositioning patients – Steep Trendelenburg patient position present risk for intraoperative injury. Injury prevention begins with awareness. Several mitigations can be deployed including; anesthesia administered crystalloids to reduce the risk for neural edema, surgeons should use the least amount of pneumoperitoneum needed for the surgery, and using the least amount of Trendelenburg needed for the procedure. The nursing team should monitor the patient position. Second timeouts involving checking patient positioning and making adjustments based on the patient physiological and physical status have been proposed for cases taking longer than 4 hours. It is standard for the nursing staff to check the safety of patient position during the case every hour when feasible. Introducing pauses for positioning checks and relieving Trendelenburg for even brief periods of time can reduce the risk for the most common injuries sustained while patients are in this position.4
Trendelenburg Position vs. Reverse Trendelenburg Position

A modified version of Trendelenburg, Reverse Trendelenburg position is used for laparoscopic surgeries including gallbladder, biliary tract, and stomach procedures, as well as head and neck surgeries. In Trendelenburg, the patient’s head is positioned down, and feet positioned up. In Reverse Trendelenburg, their head is up, and feet are positioned down.
Conclusion
Positioning a patient for a surgical procedure involves reducing risk of injury and increasing comfort. The Trendelenburg position allows a surgeon greater access to pelvic organs, helpful for procedures like colorectal, gynecological, and genitourinary surgery. As with all surgical positions, risks must be assessed prior to positioning a patient in Trendelenburg position. For example, risks to a patient while in Trendelenburg include diminished lung capacity, tidal volume and pulmonary compliance, venous pooling toward the patient’s head, and sliding and shearing. Trendelenburg position should be avoided for extremely obese patients.
References
1 Ghomi A, Kramer C, Askari R, Chavan NR, Einarsson JI. Trendelenburg position in gynecologic robotic-assisted surgery. J Minim Invasive Gynecol. 2012;19(4):485-489. doi:10.1016/j.jmig.2012.03.019
2 Guideline for positioning the patient. (2017). AORN Journal, 105(4), P8-P10. doi:10.1016/s0001-2092(17)30237-5
3 https://www.apsf.org/article/obesity-and-robotic-surgery/
4 Zillioux JM, Krupski TL. Patient positioning during minimally invasive surgery: what is current best practice? Robot Surg. 2017;4:69-76. Published 2017 Jul 14. doi:10.2147/RSRR.S115239
Knowledge Center Category List
| FOLLOW US | |
|---|---|
|
|
|
|
|
|
|
|
|
|
|
|


