Knowledge Center
October 2, 2023
The Hazards of Surgical Smoke in the OR
Learn about the dangers of surgical smoke in the operating room (OR) and how to protect yourself and your patients. Our in-depth guide covers the health risks, regulatory requirements, and best practices for surgical smoke control. Discover the latest industry insights on this critical topic.
What are the hazards of surgical smoke in the Operating Room?
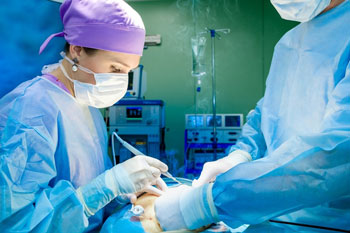
While patient care in the operating room is the number one priority of the surgical staff, the safety and care of the staff are equally important. Surgeons and their supporting staff can encounter biological and electrical hazards in each case they attend. Still, Surgical Smoke Hazards, in particular, can have short-term and long-term effects on the surgeon and their staff if not managed appropriately.
Surgical Smoke is found in almost every OR today. Ensuring the safe elimination of this smoke plume during a surgical procedure and taking the appropriate protective measures can guard the health and safety of the surgical staff and patients.
In this article, you will learn:
- What is Surgical Smoke?
- Hazards of Surgical Smoke
- Regulatory Framework for Surgical Smoke
- Solutions for Controlling Surgical Smoke
What is Surgical Smoke?
What is surgical smoke, and how is it produced?
Surgical smoke plume is a potentially dangerous by-product generated from the use of lasers, electro-surgical pencils, ultrasonic devices, and other surgical energy-based devices. As these instruments cauterize or burn vessels and destroy tissue, vaporized fluids, including blood, create a gaseous material called a surgical smoke plume.
The Composition of Surgical Smoke
The composition or chemical makeup of this smoke plume is what makes the smoke so dangerous. The plume comprises 95% water and 5% additional matter. The other 5% matter is potentially hazardous to the surgical staff and patients.
Chemical Component
The chemical component of surgical smoke plumes contains over 80 different toxic chemicals and by-products. Some of these components have documented harmful health effects, such as the following:
| Chemical Name | Common Use |
|---|---|
| Perchloroethylene | It is most commonly used as a main component in dry cleaning fluid. |
| Hydrogen cyanide | A neurotoxin used in the production of plastic and chemical weapons. |
| Toluene | A solvent that is similar to paint thinner and is a known carcinogen. |
| Formaldehyde | It is a chemical used to preserve surgical specimens and can be found in embalming fluid. |
| Ethylbenzene | It is most used in the manufacture of Styrofoam. |
| Benzene | It is a chemical used to manufacture plastics and is a known Carcinogen. |
Biological and Physical Components
Along with the chemical toxins, biological and physical components make up surgical smoke plumes that add to the overall risk factors for inhalation.
The biological matter of the plume can include blood with potential infectious viruses and bacteria. Since surgical smoke comprises approximately 95% water vapor, it creates a viable carrier for bacteria and viruses, which can transfer infectious diseases.
Evidence of an airborne virus transmitted within a surgical smoke plume is documented.
The different types of smoke produced in the Operating Room
- Electrocautery smoke
- Laser smoke
- Ultrasonic scalpel smoke
- Harmonic scalpel smoke
- Suction irrigation smoke
What are the hazards of surgical smoke?
Health risks for patients
There are associated hazards to patients when they are exposed to surgical smoke. The evidence demonstrates that the risks of surgical smoke exposure to the patient are:
- Reduced visibility of the surgical site during the procedure
- Potential delays during the procedure
- Absorption and excretion of smoke by-products and port site metastasis
Health risks for surgical staff
The synergistic and antagonistic interactions of aldehydes, benzene, toluene, ethylbenzene, xylene, ozone, and dioxins have not been studied and are difficult to predict. The researchers concluded that surgical smoke should be evacuated to protect the OR team from the toxic, possibly carcinogenic, mutagenic, and genotoxic effects.
Chemical Hazards

In a study to determine the chemical composition of surgical smoke, samples were collected of surgical smoke generated by electrocautery during colorectal surgery. The sampling tube was attached near the end of the electrocautery pencil or held in the plume above the pencil.
The electrocautery smoke contained significant benzene, ethyl benzene, styrene, carbon disulfide, and toluene. Benzene, a known carcinogen, was detected in significant quantities. The substances detected can cause eye irritation, dermatitis, central nervous system effects, and hepatic and renal toxicity.
Carcinogenicity of surgical smoke
Studies suggest that malignant cells can be aerosolized when the ultrasonic scalpel is used on tumor-bearing tissue and may be the reason for tumor recurrence at a port site remote from the original tumor.
The researchers concluded that smoke from an ultrasonic scalpel may contain viable tumor cells, and there is a theoretical risk of transfer of the viable tumor cells to anyone close to the surgical procedure.
Respiratory and skin irritation caused by surgical smoke
Due to the toxic chemical components found in surgical smoke, the respiratory system is negatively affected, but also with more severe conditions such as asthma or pneumonia. The size of the particles in the surgical smoke directly influences the type of adverse respiratory health effects experienced by the perioperative team.
Potential risks of infection transmission through surgical smoke
Viable bacteria exist within the laser smoke plume generated during laser resurfacing. Additional research is needed to define the exposure risk associated with patients who have hepatitis, HIV, and antibiotic-resistant bacteria.
Regulatory Framework for Surgical Smoke
Overview of the current regulatory landscape
The most recent version of the American National Standards Institute Z136.3 (2011) states that airborne contaminants from laser surgery SHALL be controlled. Also, it notes that electrosurgical devices produce the same type of airborne contaminants as lasers. Many organizations and agencies are making their recommendations more powerful by changing the verb from “should” to the more powerful word “shall” to help encourage compliance.
Guidelines for controlling surgical smoke
Several national and international organizations address standards concerning patients' and healthcare workers’ exposure to hazardous materials and surgical smoke.
According to the National Institute of Occupational Safety and Health /Centers for Disease Control, ventilation techniques include a combination of general room and local exhaust ventilation (LEV):
- Portable smoke evacuators
- Room suction systems
NIOSH/CDC recommends that:
- The smoke evacuator or room suction hose nozzle inlet must be kept within 2 inches of the surgical site.
- The smoke evacuator should always be ON (activated) when a plume is present.
- Healthcare workers should follow standard precautions.
Click to learn more about the surgical smoke legislation and policy
Solutions for Controlling Surgical Smoke
Surgical smoke evacuation systems
One of the most effective methods of removing the hazards of surgical smoke plumes is using Smoke Evacuation Systems. These systems remove the plume at its surgical site source by using a tube attached to the accessory or device creating the plume. Connecting it to the surgical site (approximately within 2 inches of the plume source), about 99.9% of 0.12-micron sizes or larger can be removed from the environment before inhalation.
The system usually contains a series of filters allowing filtration down to the micron size to ensure even the smallest particulates can be captured.
Smoke evacuation unit:
Generates suction and houses filters.
Filters:
They filter surgical smoke from the air as it passes through the Unit.
Tubing:
Transport surgical smoke from the surgical site to the Unit.
Electrocautery pencils with integrated smoke evacuation:
They allow the STERIS smoke evacuation system to collect and filter smoke right at the incision site. These patented electrocautery pencils work with other surgical smoke evacuation systems.
Shrouds:
Transport surgical smoke from the surgical site to the Unit.
Learn about the STERIS Smoke Evacuation System
Surgical masks:
With surgical masks, the surgical staff helps to control the transfer of microorganisms from the staff to the patient. However, it protects the surgeon and staff from inhaling surgical smoke plumes. The masks' filtration or particulate can vary, but even the smallest particle size masks can’t eliminate viruses from being inhaled.
Proper OR ventilation:
Another safeguard against surgical smoke plume exposure and inhalation is to ensure the OR has proper ventilation. According to the AORN organization, the OR should be at least 15 air exchanges per hour. All ORs should maintain positive air pressure to ensure potentially contaminated air is being pulled away from the room.
Training and education for surgical staff
Educating perioperative team members about the hazards of surgical smoke is essential. Take advantage of all available resources in designing education to increase awareness about smoke evacuation practices. Leadership support is also essential for implementing, maintaining, and enforcing a smoke evacuation program.
Conclusion
Summary of hazards of surgical smoke in the operating room
Importance of implementing solutions for controlling surgical smoke
Regularly updated hazard assessments for operational exposure are indispensable. Close cooperation should be established between occupational safety specialists and occupational health physicians. The implementation of OH&S recommendations in Standard Operating Procedures (SOP) is also recommended.
Surgeons and assistant staff should be better informed about the possible health risks of surgical smoke and its prevention. Awareness raising can occur through regularly updated instruction and other formalized training, such as a facility-based initiative, and manufacturers of smoke evacuation devices should be invited to support regular onsite training.
Contributors

Lena Fogle BSN, RN, CNOR
Senior Director Global Clinical Solutions, STERIS Healthcare
Lena is a seasoned healthcare leader with extensive experience leading complex perioperative environments and new program development, continuous process improvement, clinical outcomes, operational excellence, and stakeholder experience.
Related Resources
Article References
1 Okoshi, K.; Kobayashi, K.; Kinoshita, K.; Tomizawa, Y.; Hasegawa, S.; Sakai, Y. Health risks associated with exposure to surgical smoke for surgeons and operation room personnel. Surg. Today 2015, 45, 957–965. [CrossRef] [PubMed]
2 Andréasson SN, Anundi H, Sahlberg B, et al. Peritonectomy with high voltage electrocautery generates higher levels of ultrafine smoke particles. Eur J Surg Oncol. 2009;35(7):780-784.
3 Ball K. Compliance with surgical smoke evacuation guidelines: implications for practice. AORN J. 2010;92(2):142-149
4 Calero L, Brusis T. Laryngeal papillomatosis—first recognition in Germany as an occupational disease in an operating room nurse. Laryngorhinootologie. 2003;82(11):790-793.
5 Capizzi PJ, Clay RP, Battey MJ. Microbiologic activity in laser resurfacing plume and debris. Lasers Surg Med. 1998;23(3):172-174.
6 Dobrogowski M, Wesolowski W, Kucharska M, Sapota A, Pomorski LS. Chemical composition of surgical smoke formed in the abdominal cavity during laparoscopic cholecystectomy—assessment of the risk to the patient. Int J Occup Med Environ Health. 2014;27(2):314-325.
7 Dobrogowski M, Wesolowski W, Kucharska M, et al. Health risk to medical personnel of surgical smoke produced during laparoscopic surgery. Int J Occup Med Environ Health. 2015;28(5):831-840.
8 Guideline for a Surgical Smoke Safety. In: Guidelines for Perioperative Practice. Denver, CO: AORN, Inc; 2017:477-506.
9 Hallmo P, Naess O. Laryngeal papillomatosis with human papillomavirus DNA contracted by a laser surgeon. Eur Arch Otorhinolaryngol. 1991;248(7):425-427.
10 Hill DS, O'Neill JK, Powell RJ, Oliver DW. Surgical smoke—a health hazard in the operating theatre: a study to quantify exposure and a survey of the use of smoke extractor systems in UK plastic surgery units. J Plast Reconstr Aesthet Surg. 2012;65(7):911-916.
11 In SM, Park DY, Sohn IK, et al. Experimental study of the potential hazards of surgical smoke from powered instruments. Br J Surg. 2015;102(12):1581-1586.
12 Ishihama K, Sumioka S, Sakurada K, Kogo M. Floating aerial blood mists in the operating room. J Hazard Mater. 2010;181(1-3):1179-1181.
13 Jewett DL, Heinsohn P, Bennett C, Rosen A, Neuilly C. Blood-containing aerosols generated by surgical techniques: a possible infectious hazard. Am Ind Hyg Assoc J. 1992;53(4):228-231.
14 Johnson GK, Robinson WS. Human immunodeficiency virus-1 (HIV-1) in the vapors of surgical power instruments. J Med Virol. 1991;33(1):47-50.
15 Mihashi S, Ueda S, Hirano M, Tomita Y, Hirohata T. Some problems about condensates induced by CO2 laser irradiation. Paper presented at: Fourth International Society for Laser Surgery; November 1981; Tokyo, Japan.
16 Näslund Andréasson S, Mahteme H, Sahlberg B, Anundi H. Polycyclic aromatic hydrocarbons in electrocautery smoke during peritonectomy procedures. J Environ Public Health. 2012;2012:929053.
17 Petrus M, Bratu AM, Patachia M, Dumitras DC. Spectroscopic analysis of surgical smoke produced in vitro by laser vaporization of animal tissues in a closed gaseous environment. Romanian Reports in Physics. 2015;67(3):954-965.
18 Petrus M, Matei C, Patachia M, Dumitras DC. Quantitative in vitro analysis of surgical smoke by laser photoacoustic spectroscopy. J Optoelectron Adv M. 2012;14(7-8):664-670.
19 Rioux M, Garland A, Webster D, Reardon E. HPV positive tonsillar cancer in two laser surgeons: case reports. J Otolaryngol Head Neck Surg. 2013;42:54.
20 Sagar PM, Meagher A, Sobczak S, Wolff BG. Chemical composition and potential hazards of electrocautery smoke. Br J Surg. 1996;83(12):1792.
21 Tomita Y, Mihashi S, Nagata K, et al. Mutagenicity of smoke condensates induced by CO2-laser