Knowledge Center
May 31, 2023
Operating Room Sterilization: A Complete Guide to Air Quality
Global events have raised awareness about contamination in recent years, yet surgical site infections (SSI) remain the most common and costly of all hospital-acquired infections (HAI). An estimated 157,500 SSIs occur annually, representing 22% of total HAI. According to a study on preventing surgical-site infections1, 98% of SSI can be attributed to airborne particulate.
Airborne particles such as skin cells (squames) may carry bacterial loads and settle directly on a wound or be transferred to a wound after from a surgeon’s hands or the surgical instruments themselves. Since the primary cause of SSI is chiefly attributable to airborne contamination, air quality in the operating room (OR) should be of utmost importance in promoting patient and staff safety.
What you’ll learn in this article:
- The impact of air delivery and filtration on operating room contamination
- Using in-duct and ceiling-mounted air and surface sanitization systems to fight microorganisms
- The four types of ultraviolet (UV) light systems for room sterilization and the impact on OR uptime
LEARN ABOUT CLEANSUITE® CEILING SYSTEM
Air Quality in Operating Room Design
From an OR design perspective, there are ways to help mitigate the risks associated with airborne contamination. The goal is to guide or neutralize airborne particulate away from the sterile field and instrument tables. Such solutions include unidirectional air delivery and filtration systems, in-duct or ceiling-mounted air, and surface sanitization systems.
Unidirectional Air Delivery and Filtration
In the U.S., OR air quality is regulated by three organizations: the American National Standards Institute (ANSI); the American Society of Heating, Refrigerating and Air-Conditioning Engineers (ASHRAE); and the American Society for Healthcare Engineering (AHSE). The combined ANSI/ASHRAE/ASHE Standard 170-2021, Ventilation of Healthcare Facilities, provides a granular approach to air cleanliness based on the “function of space.” Thus, operating rooms require positive pressure, a minimum of 20 air changes per hour (ACH), with a minimum of four outdoor changes per hour. The standard specifies a minimum effective reporting value for air filter efficiency (MERV 16) but does not recommend a type of air delivery system.
In February 2014, ASHRAE Journal published a peer-reviewed article, “Improving Operating Room Contamination Control.”2 The study intended to analyze how turbulent air might contribute to airborne particulate settling in a surgical wound. The study evaluated three fundamental design concepts for ceiling-mounted OR air delivery systems: air curtain, multi-diffuser array, and prefabricated single-large diffuser.
Air Curtain
Creating an air curtain utilizes a high-velocity slot and laminar flow diffuser around the perimeter of the sterile field to create a barrier of air that protects the sterile field from outside contaminants. Air curtain technology originated in the 1950s and has since been replaced by the multi-diffuser array in most hospitals.
Multi-Diffuser Array
This method uses multiple laminar flow diffuser panels set into an array in the ceiling. Multi-diffuser technology originated in the 1960s, and most ORs in North America still use this system.
Prefabricated Single-Large Diffuser
A single-large diffuser is an advanced method of gapless delivery of unidirectional air in a controlled fashion. This design originated in the cleanroom sector in the 1990s and has been commercially available to hospitals since the 2010s. Systems such as CLEANSUITE® use room-side high-efficiency particulate absorbing (HEPA) filtration, which exceeds MERV 16, to significantly reduce the amount of airborne particulate within the trunk line, from the air handler to the OR suite.
Using a computational fluid dynamics (CFD) particle trace, the ASHRAE study concluded that the air curtain and multi-diffuser array designs created turbulent zones without airflow delivery beneath certain areas. In contrast, the prefabricated single-large diffuser reduced the turbulent zones. In the figure below, the particle trace from a multi-diffuser array system (left) shows a turbulent dispersion of contaminants in the operating theatre, compared to the efficient and controlled movement of particles away from the sterile field in a prefabricated single-large diffuser (right).
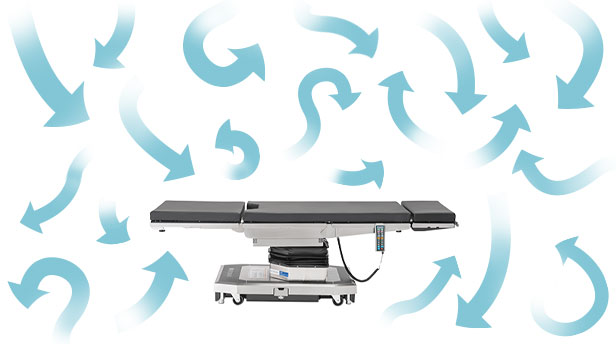
Multi-Diffuser Array

Prefabricated Single-Large Diffuser
In-duct and Ceiling-Mounted Air and Surface Sanitization Systems
In addition to advanced air delivery methods, many health systems are exploring in-duct or ceiling-mounted air and surface sanitization systems to augment their routine cleaning and decontamination procedures. Hospitals use UV light in these systems to create continuous passive disinfection of the air and targeted surfaces in the operating theatre.
Germicidal ultraviolet light in the UV-C wavelength of roughly 290 to 200 nanometers has been used extensively in various heating, ventilation, and air conditioning/refrigeration (HVAC/R) systems since the 1990s. Technology with UV-C light can be an effective tool for infection prevention because it disrupts the DNA of microorganisms and prevents them from replicating. Its efficacy against different organisms (e.g., viruses, bacteria, fungi, spores) is a product of exposure time, intensity, and distance from the UV source to the target. In other words, a greater intensity or longer exposure time is necessary to eliminate a given microbe the further away an organism is from the UV source.
UV-C Efficacy = Intensity x Exposure Time x Distance
Hospitals have four different UV light systems that can be deployed in an OR setting to reduce microbial contamination in the air and on surfaces after routine manual cleaning and disinfection practices are observed.
-
Mobile UV Devices: Mobile UV devices are systems built on wheels located in the OR near high-touch surfaces. These units are generally 254 nanometers in wavelength and effectively decontaminate targeted room components when a clear line of sight is available. Any obstruction between the device and the target will require the user to reposition the device or remove the obstacle to achieve proper exposure.
Limitations: Patients and staff cannot be in the room during treatment. Long-term exposure to UV-C energy may also discolor and embrittle equipment and materials in the room.
-
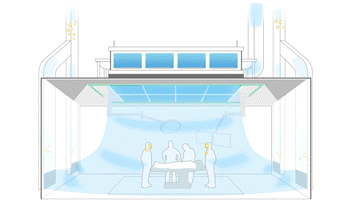
Ceiling-Mounted Systems: Ceiling-mounted systems are incorporated in the OR ceiling grid, usually outside the sterile field perimeter. Such systems may use either 254 nm or 405 nm wavelength energy. Much like mobile systems, they effectively treat various targeted room components in the line-of-sight treatment.
Limitations: Patients and staff can be in the room during treatment, but only under low-intensity conditions with full use of personal protective equipment (PPE), including no exposed skin and complete eyewear protection. Though it is typical in orthopedic procedures for total joint replacements, this level of gowning may be uncomfortable for the staff to wear in non-ortho procedures. Ceiling fixtures are limited by obstructions (e.g., ceiling-mounted lights, surgical booms, c-arms) which must be moved to achieve proper efficacy in the targeted area. Like mobile UV devices, long-term exposure to the wavelength energy from these systems may yellow and weaken the material of different OR equipment.
-
In-Duct UV Systems: In-duct UV-C systems treat the supply air before it enters the OR. Typically, a sealed reaction chamber device is mounted inside the duct, and as air passes through the machine, it neutralizes microbial contaminants in the air stream. These systems effectively supply clean air from the air handler to the OR delivery system. Patients and staff can be in the room during treatment without additional PPE.
Limitations: These systems do not treat room materials or airborne skin cells that the patient or staff has shed within the room.
-
In-Duct Hydroxyl Generator Systems: In-duct hydroxyl generator systems utilize multiple wavelengths of ultraviolet energy to produce reactive oxygen species known as hydroxyls. Airborne hydroxyls are ideal sanitizing agents which reduce pathogens and neutralize volatile organic compounds (VOC) and a broad range of chemicals. Hydroxyl generators such as the PYURE Air and Surface Sanitization System mimic how natural sunlight sanitizes our outdoor environment by safely generating and dispersing hydroxyls and organic oxidants indoors.
Atmospheric hydroxyls are natural-occurring molecules produced by the action of the sun’s ultraviolet energy on oxygen and water in our atmosphere. The hydroxyls are a natural oxidant and safe for patients and staff to be present during treatment without additional PPE. The system treats airborne contaminants during active surgery at the most critical time for patients and staff. The system can run continuously and year-round, providing the potential for maximum surgical uptime. There is no need to reposition a device or exit the OR during treatment. An added benefit is that hydroxyls help mitigate odors caused by surgical smoke and cauterized tissues.
Limitations: None. If desired, the solution is fully scalable from the sterile field space to the entire room and building.
Summary
The level of awareness for airborne contamination has increased in light of recent global events, and the invisible threat has become much more visible. Progressive healthcare systems are actively addressing operating room air quality during the design of new construction or renovation projects. Using prefabricated single-large diffuser OR air delivery systems such as CLEANSUITE, combined with in-duct hydroxyl generator systems such as PYURE, gives innovative health systems a clear advantage in improving air quality.
Contributors

Jim Dacek
MBA, LEED Green Associate
Jim is a seasoned product development leader with extensive experience in adapting progressive cleanroom processes and technologies to further enhance patient and staff safety/satisfaction by transforming traditional healthcare spaces.
Related Resources
Article References
1 Chauveaux, Dominique. Preventing surgical-site infections: Measures other than antibiotics. Orthopaedics & Traumatology: Surgery & Research, Volume 101, Issue 1, Supplement, Pages S77-S83. https://www.sciencedirect.com/science/article/pii/S1877056814003272. 2015.
2Wagner, Jennifer A., PH.D; Schreiber, Kevin J.; Cohen, Ralph, P.E. Improving Operating Room Contamination Control. ASHRAE Journal. https://www.ashrae.org. 2014.




