Knowledge Center
May 31, 2018
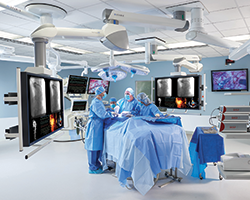
What is a Hybrid Operating Room?
Benefits of Hybrid Operating Room?
A Hybrid Operating Room is an advanced procedural space that combines a traditional operating room with an image guided interventional suite. This combination allows for highly complex, advanced surgical procedures. Not only are the rooms combined but the teams are combined to form a multi-disciplinary group of clinicians prepared to meet the complex needs of patients.
A Hybrid OR is an aseptic environment that combines surgical equipment, instruments, surgical tables, OR Lights, equipment management systems, and surgical booms along with fixed advanced imaging systems, offering the capability to perform combined image-guided procedures with minimally invasive procedures. These state-of-the-art spaces also allow for the combination of image guided surgery with open procedures. Finally, if the need arises to convert a minimally invasive surgery to an open procedure, these spaces allow for a smooth transition to an open procedure by providing all the necessary capability and personnel in one space.1 Additionally, this technology has led to the development of new procedures that enable greater options for patients with complex disease states.
Explore our Hybrid Operating Room Solutions
Patient Safety
Patients typically experience a shorter recovery time following a procedure in a Hybrid OR, due to less stress from multiple surgeries. Additionally, patients typically have a shorter length of stay at the hospital because they don't have to recover from multiple procedures, and don't require as many patient management resources.1
Hybrid ORs allow for the ability to attempt a minimally invasive surgery procedure that was once considered unsafe due to the potential of the procedure rapidly converting to an open procedure that requires an equipped environment, specific equipment and personnel.2
Staff Efficiency
A hospital that utilizes a Hybrid OR avoids duplicated equipment, resources, space, supplies and staff allocations to each space. With a Hybrid OR, staff saves time with surgeries as procedures can be booked as one procedure versus two separate procedures. Additionally, a Hybrid OR gives the surgeon the ability to revise the traditional treatment plan and work in the same surgical suite on procedures requiring multiple interventions or modalities.2
Cost Effective
Because a Hybrid OR features surgical equipment and imaging in one location, equipment or technology troubleshooting is only needed in one place versus two. Also, a Hybrid OR frees space for standard operating rooms and interventional suites.1
Hybrid ORs help improve patient outcomes, speed patient recovery time and reduce length of patient stays, decreasing cost for the healthcare organization.2
Hybrid Operating Room Applications
Due to their flexible design and multi-disciplinary resources, more and more procedures are being performed safely and efficiently in Hybrid ORs, including cardiac procedures that were previously performed in cath labs.1
Minimally Invasive Surgery
Hybrid ORs allow for many minimally invasive procedures such as Transcatheter Aortic Valve Replacement (TAVR), and Endovascular Aneurysm Repair (EVAR).
Advanced Medical Procedures
Various advanced medical procedures can be performed in a Hybrid OR.
Planning a Hybrid Operating Room
A Hybrid OR involves planning and design with the collaboration of personnel throughout the hospital system, including but not limited to administration, neurosurgeons, cardiologists, facility planners, anesthesiologists, nurses, surgical technologists, and Information Technology (IT) staff.1
Workflow
The arrangement of medical equipment, operating room supplies, and traffic patterns are workflow factors that all must be considered when planning a Hybrid OR.
Challenges of Designing a Hybrid Operating Room
There are a variety of challenges when planning and designing a Hybrid OR, including equipment integration, patient flow, capital expense, vendor coordination, radiation safety, space and workflow requirements. Successful Hybrid operating room projects have several factors in common, including multidisciplinary project team, clinician involvement upfront and throughout, early identification of vendor partners with a proven track record of hybrid room design and equipment outfitting that is customized to meet the facility's vision.
Space Requirements
The average size of a Hybrid Operating Room is 1,100 square feet. A standard OR, on average, is roughly 600 square feet. When planning a Hybrid OR, ceiling heights and ceiling support structures should be evaluated and considered. A positive pressure laminar airflow system is recommended to maintain an OR level of sterility, specifically if space will be used for neurosurgery and orthopedic trauma procedures.3
Implementation Time
The project time-line from the initial decision to build a hybrid OR to the completion of the project will depend on whether an existing space is being retrofitted or if it is a new construction project. New construction can be up to 2 years, while a retrofitting project will be somewhat less depending on the existing structure. A carefully planned project that includes bringing together key stakeholders and trusted vendors early in the project can significantly shorten the time and reduce the risk along the way. Making vendor and design decisions up front will assist in the organization and success of the project.
Staff Training
The multidisciplinary team includes clinicians trained in their specialty. Additional training will include new workflow of the Hybrid OR, cross training on equipment so personnel can assist one another as cases move from one phase to another, and training on any new procedure contemplated.
Requirements for a Hybrid Operating Room
In addition to all standard operating room equipment, Hybrid Operating Rooms require fixed advanced imaging systems, control rooms, advanced integration with multiple monitors, separate equipment storage room, and high band width for many sources and destinations. They will also require a wide array of diagnostic equipment from ultrasounds to recording systems.
1. https://www.ormanager.com/hybridor/article3/
2. The Cardiovascular Hybrid OR-Clinical & Technical Considerations | CTSNet. (n.d.). Retrieved from http://www.ctsnet.org/article/cardiovascular-hybrid-or-clinical-technical-considerations
3. Schaadt, J., & Landau, B. (2013). Hybrid OR 101: A Primer for the OR Nurse. AORN Journal, 97(1), 81-100. doi:10.1016/j.aorn.2012.10.009


